What Is The Muscle That Subdivides The Ventral Body Cavity
listenit
Apr 02, 2025 · 6 min read
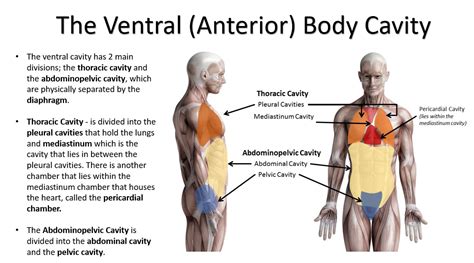
Table of Contents
What is the Muscle That Subdivides the Ventral Body Cavity?
The human body is a marvel of intricate design, with various systems working in harmony to maintain life. One crucial aspect of this design is the organization of internal spaces, or body cavities. These cavities house and protect vital organs, allowing them to function optimally. A key player in the organization of the ventral body cavity, the large, anterior cavity of the trunk, is the diaphragm. This article will delve deep into the diaphragm's anatomy, function, and clinical significance, providing a comprehensive understanding of its role in subdividing this crucial body space.
The Ventral Body Cavity: A Broad Overview
Before focusing on the diaphragm, it's essential to understand the ventral body cavity itself. This vast space is located at the front of the body and is further divided into two main cavities: the thoracic cavity and the abdominopelvic cavity. This subdivision is paramount for the protection and independent functioning of the organs within each.
Thoracic Cavity: The Upper Compartment
The thoracic cavity, situated superiorly, houses vital organs responsible for respiration and circulation. These include the:
- Lungs: The primary organs of respiration, responsible for gas exchange.
- Heart: The central pump of the circulatory system, driving blood throughout the body.
- Thymus gland: An important part of the immune system.
- Major blood vessels: Including the aorta, vena cava, and pulmonary arteries and veins.
- Esophagus: The tube connecting the pharynx to the stomach.
- Trachea: The windpipe, carrying air to and from the lungs.
Abdominopelvic Cavity: The Lower Compartment
Inferior to the thoracic cavity lies the abdominopelvic cavity, which is further subdivided into the abdominal and pelvic cavities, though there is no physical separation between them. This cavity houses the digestive, urinary, and reproductive systems. Key organs include:
- Stomach: Responsible for initial digestion.
- Small intestine: Where the majority of nutrient absorption occurs.
- Large intestine: Involved in water absorption and waste elimination.
- Liver: Performs numerous metabolic functions.
- Gallbladder: Stores bile produced by the liver.
- Pancreas: Produces digestive enzymes and hormones.
- Kidneys: Filter blood and produce urine.
- Spleen: Plays a crucial role in the immune system.
- Urinary bladder: Stores urine.
- Reproductive organs: Including the ovaries, uterus, and testes.
The Diaphragm: The Master Divider
The diaphragm, a dome-shaped, sheet-like muscle, forms the crucial boundary between the thoracic and abdominopelvic cavities. Its unique structure and function are central to respiration and maintaining the integrity of these vital body compartments.
Anatomy of the Diaphragm
The diaphragm's anatomical features are intricately designed to facilitate its role in breathing. Its components include:
- Central Tendon: A strong, aponeurotic central region where the muscle fibers converge.
- Muscular Portions: The diaphragm's muscle fibers arise from several points of origin:
- Sternal Part: Originates from the posterior surface of the xiphoid process of the sternum.
- Costal Part: Originates from the inner surfaces of the lower six ribs and their costal cartilages.
- Lumbar Part: Originates from the lumbar vertebrae via two crura (right crus and left crus), which are tendinous structures.
- Medial and Lateral Arcuate Ligaments: These ligaments connect the crura to the quadratus lumborum muscle.
Innervation of the Diaphragm
The phrenic nerves, originating from the cervical spinal cord (C3-C5), provide motor innervation to the diaphragm. This unique innervation is crucial, as it allows for diaphragmatic function even if spinal cord injuries occur below the cervical region. Sensory innervation to the diaphragm is more complex, coming from both the phrenic nerves and intercostal nerves.
Blood Supply of the Diaphragm
The diaphragm's blood supply is robust, ensuring adequate oxygen and nutrient delivery to its working muscles. This includes contributions from:
- Pericardiophrenic arteries: Branches of the internal thoracic artery.
- Musculophrenic arteries: Branches of the internal thoracic artery.
- Superior phrenic arteries: Branches of the thoracic aorta.
- Inferior phrenic arteries: Branches of the abdominal aorta.
These arteries, along with the corresponding veins, maintain the continuous supply and removal of blood crucial for proper diaphragm functioning.
The Diaphragm's Role in Respiration
The diaphragm's primary function is its role in respiration, specifically inhalation. During inhalation:
- The diaphragm contracts, causing its dome to flatten and move inferiorly.
- This downward movement increases the volume of the thoracic cavity.
- The increase in volume decreases the intrathoracic pressure.
- Air rushes into the lungs to equalize the pressure difference.
Exhalation is primarily passive, involving the relaxation of the diaphragm and elastic recoil of the lungs. However, forceful exhalation requires the action of abdominal muscles.
Clinical Significance of the Diaphragm
The diaphragm's crucial role in respiration and its anatomical position make it a clinically significant structure. Several conditions can affect the diaphragm, including:
- Diaphragmatic hernia: A condition where abdominal organs protrude into the thoracic cavity through a defect in the diaphragm. This can cause respiratory distress and potentially life-threatening complications. Types of diaphragmatic hernias include congenital diaphragmatic hernia (present at birth) and acquired diaphragmatic hernia (develops later in life due to trauma or weakness).
- Diaphragmatic paralysis: Weakening or paralysis of the diaphragm, often due to nerve damage, leading to impaired breathing. This can be caused by various factors including trauma, surgery, or neurological conditions. Symptoms can vary depending on the severity of the paralysis.
- Hiatal hernia: A type of diaphragmatic hernia where the stomach protrudes through the esophageal hiatus, the opening in the diaphragm where the esophagus passes. This can cause heartburn and gastroesophageal reflux disease (GERD).
- Diaphragmatic eventration: The upward displacement of the diaphragm, often due to paralysis or weakening of one side. This compromises respiratory function.
These conditions highlight the diaphragm's importance for maintaining respiratory health and overall body function. Accurate diagnosis and timely intervention are essential to mitigate potential health risks.
Diaphragm and other Muscles Supporting Respiration
While the diaphragm is the primary muscle of respiration, it works in conjunction with other muscles to facilitate efficient breathing. These include:
- External intercostal muscles: These muscles located between the ribs help expand the chest cavity during inhalation.
- Internal intercostal muscles: These muscles assist in forced exhalation.
- Abdominal muscles: Muscles such as the rectus abdominis, external oblique, internal oblique, and transversus abdominis are essential for forceful exhalation by compressing the abdominal contents and pushing the diaphragm upwards.
- Accessory muscles of respiration: These muscles become more involved in breathing during strenuous activity or respiratory distress. Examples include the sternocleidomastoid, scalenes, and pectoralis minor.
Conclusion: The Diaphragm's Indispensable Role
The diaphragm is more than just a muscle; it's a vital anatomical structure that plays a critical role in separating the thoracic and abdominopelvic cavities and enabling respiration. Its intricate anatomy, innervation, and blood supply all contribute to its essential function. Understanding the diaphragm's anatomy and its clinical significance is essential for healthcare professionals and anyone seeking a deeper understanding of human physiology. Disruptions to its normal function can have significant consequences for respiratory health, emphasizing the need for proper care and timely interventions when problems arise. Further research continues to explore the intricacies of diaphragmatic function and its role in various physiological processes.
Latest Posts
Latest Posts
-
1 4 As An Improper Fraction
Apr 03, 2025
-
What Is The Inverse Of X 2
Apr 03, 2025
-
What Is The Charge Of Chlorine
Apr 03, 2025
-
Area Of A Circle With A Radius Of 7
Apr 03, 2025
-
Find The Slope Of The Line Perpendicular
Apr 03, 2025
Related Post
Thank you for visiting our website which covers about What Is The Muscle That Subdivides The Ventral Body Cavity . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
